How effective are the available methods to treat drug addiction in the country? The majority of the drug addiction treatment programs offered by accredited drug rehab centers in the U.S. do not have a standardized approach to measuring their success rates.
Treatment engagement is one of the well-established performance measures for the success of substance use disorder programs and for rehab centers.
Success rates are also often assessed by evaluating the number of people who relapsed to drug use after leaving a given drug rehab center or by comparing the number of relapses to the number of cases of ongoing sobriety.
Some drug rehab centers measure the success of their addiction treatment programs by looking at the number of patients who were able to fully complete their specific programs. Several other rehabilitation facilities will take into account the rates of sobriety of the patients immediately after they have been cleared to leave the treatment center.
Additional ways to measure the success rates of a drug rehab center include evaluations or studies, which are usually conducted internally or by the parent companies of the organizations that are offering the addiction treatment services.
There are numerous addiction treatment programs, drug detox and rehab centers that claim to have nearly perfect success rates, but such claims are usually related to the fact that there are flexible criteria to measuring success; consequently, these assertions can be misleading.
New medical specialty
One of the potential explanations for the fact that there aren’t precise methods to track the success rates of the drug rehab centers and the addiction treatment programs in the country is that addiction medicine is a fairly new medical sub-specialty, at least officially.
Dr. Yngvild Olsen, an addiction specialist, an at-large member of the American Society of Addiction Medicine (ASAM) Board of Directors and chair of ASAM’s Public Policy Committee, explained that the field addiction medicine was first recognized as a medical subspecialty by the American Board of Medical Specialty in the spring of 2016. The recognition, she said, was sponsored by the American Board of Preventive Medicine alongside ASAM.
Subsequently, qualified physicians were able to take an exam to officially become board certified to treat patients with substance use disorders in the fall of 2017 for the very first time.
“The workforce of physicians and other healthcare professionals who are trained and specialized to treat addiction is woefully inadequate,” Olsen said. “But it is important for us to understand that addiction medicine is a valued and a valuable profession.”
Olsen also emphasized the fact that only one in 10 U.S. residents that acknowledge they need addiction treatment have the ability to receive it, which highlights the national need for more addiction specialists.
“The opioid epidemic has really brought awareness to the issue of addiction,” she said. “There has been a lot of focus on the need for treatment. ASAM hopes that by educating the public and our physician colleagues, we can highlight that certifying more addiction medicine physicians and this new subspecialty will ensure that patients receive the professional care that they need and that they deserve.”
First steps to success
Dr. Sarah Wakeman, the head of the Substance Use Disorder Initiative at the Massachusetts General Hospital and a Harvard physician who specializes in addiction treatment, explained that the initial assessment of a person’s substance use disorder is crucial in determining their treatment outcomes.
“The earliest way we can identify [substance use disorders] is through screenings in primary care settings and in a few other settings that allow us to spot the people who have unhealthy alcohol or drug use habits before they actually develop the disease of addiction,” she said. “There are several questions that we can ask about their alcohol and drug use that can identify the people who are at high risk of developing a substance use disorder.”
Wakeman explained that if a substance use disorder is detected before it has been fully developed and healthcare providers can intervene, the patient that has been diagnosed will have much higher chances of successfully completing treatment.
“When someone actually develops a substance use disorder, we can make a diagnosis based on the criteria that are outlined on the DSM-5,” she said, referring to the Diagnostic and Statistical Manual of Mental Disorders. “There are 11 criteria and you have to meet at least two to have a diagnosis of a substance use disorder. And it is graded on how severe it is — you can have a mild, a moderate or a severe substance use disorder, depending on how many of the criteria you meet.”
The degree of someone’s drug addiction is a crucial element in determining the type of addiction treatment that person will be needing or benefitting from the most.
What do federal agencies say?
Reports from the National Institute on Drug Abuse (NIDA) affirm that success is an individual concept when it comes to drug rehabilitation; the treatment outcomes of an individual are determined by the severity of the substance use disorder that person is struggling with and by the suitability of the services and the support that has been provided.
NIDA representatives suggest that relapsing to drug use is often seen by people with substance use disorders and their loved ones as an indicator that the addiction treatment has failed — but that is not the case.
Members of the agency explained that having a substance use disorder is similar to having any other chronic disease, such as hypertension or diabetes. The fact that a chemical addiction is very similar to chronic diseases essentially means that relapsing into the habits that fulfill the condition is not just possible but very probable.
A relapse should mean that the treatment needs more adjustments or that modifications should be considered, NIDA representatives affirm; adding that for an addiction treatment program to be successful, recurrent evaluations and alterations are required.
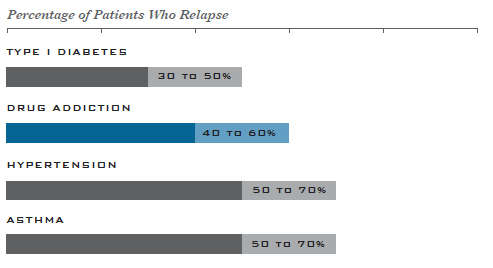
The agency also indicates that there are studies that highlight that most people who have substance use disorders benefit from remaining in treatment for extended periods of times.
Long-term addiction treatment programs not only help people stay away from drugs but are also advantageous to society due to the improvements in patients’ psychological, social and occupational abilities as well as reduced rates of criminal activities committed by those individuals.
Clinical research projects & studies
A study conducted recently by scholars from the University of Southern California has shown that people are more likely to remain sober after leaving a drug rehab center if they stay in an addiction treatment program for more than a month.
The results of the study, published in the medical journal Scientific Research, show that 55 percent of the 72 subjects who had been able to complete an addiction treatment program lasting 30 days at a rehab center remained sober one year after the program had ended. And nearly 85 percent of the subjects who stayed in the program for more than a month continued to be sober for one year after they had left the treatment center. This, the researchers stated, is further proof that the extensiveness of a drug rehab program is directly correlated to a patient’s’ abilities to successfully remain sober.
The lead author and researcher of the study, Dr. Akikur Mohammad, also highlighted that post-treatment assistance is crucial to prevent patients from relapsing. He added that there weren’t any significant discrepancies regarding drug rehab treatment results and demographic aspects.
Mohammed stated that one of the barriers patients encounter while trying to successfully recover from a substance use disorder is the fact that federal assistance for addiction treatment hardly ever covers the costs of programs that last more than a month.
Another study — published in 2016 in the Substance Abuse Journal and supported by the National Institute on Alcohol Abuse and Alcoholism — analyzed treatment engagement patterns of individuals in outpatient addiction treatment programs.
The researchers who conducted the study, from the Boston University and Brandeis University, found that the patients who participated in outpatient programs after leaving a drug rehab program were less likely to have a subsequent admittance into a drug detox center.
The researchers stated treatment engagement analysis can be a valuable method for monitoring the quality of care received by people with substance use disorders.
The bottom line
Addiction treatment works — this is a premise supported by all of the reputable medical authorities in the country, including the Substance Abuse and Mental Health Services Administration (SAMHSA).
“[Addiction] treatment is not only available but it is effective,” said Dr. Beth Han, the lead author of the latest Behavioral Health Barometer by SAMHSA and a researcher at the agency’s Center for Behavioral Health Statistics and Quality.
For treatment to be successful, it needs to meet the specific needs of each individual patient, she added.
But according to SAMHSA, the most important message to be sent to the public is that more addiction treatment services need to be made available.
The behavioral health report authored by Han shows that only 11 percent of the 850,000 U.S. residents who needed treatment for a substance use disorder involving illicit drugs received the services in an alcohol or drug rehab center, a behavioral healthcare facility or a hospital in 2015.
Addiction treatment services that have been proven to be effective, such as medication-assisted treatment for persons with opioid use disorders, also need to expand, SAMHSA representatives stated.
“We can see that the number of people receiving treatment for prescription opioid misuse has increased,” Han said. “But we hope to see that number continue to go up.”